Too Much Of A Good Thing...
Someone much more intelligent than me once said that too much of a good thing may be a bad thing. Or could be a bad thing. Or something like that. You get the idea.
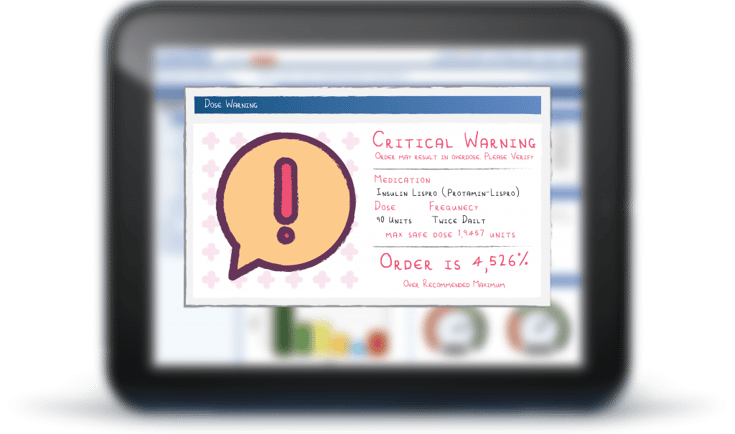
Recently, a physician asked me about an alert that he saw while ordering a medication in the hospital’s electronic health record (EHR). It looked something like this (names and details have been changed to protect the innocent!):
If you’re involved in healthcare IT, you already know that there is such a thing as alert fatigue. Doctors and nurses (in other words, humans) often become numb to the computer reminding them to do something or warning them that what they’re trying to do might be dangerous to the patient, or at least may not be the best practice.
EHR vendors and the informaticists who implement and maintain their systems have been working to combat alert fatigue via a variety of methods (maintaining the five rights of CDS, incorporating user-centered design, etc.) I’d like to point out one intervention that some may be overlooking: the proper level of numerical precision.
In the example above, the EHR is notifying the physician of two key “facts”:
- The max safe dose is 1.9457 units of insulin
- This single dose is 4,526 percent above the max safe dose
When physicians see numbers like this, they reasonably question the validity of the advice being offered. To begin with, we should consider that the ordering physician might have made a huge mistake and given 45x the safe dose. It might be that we’re going to have to have a conversation about what the safe max dose really is. Alternatively, it could be that this is a weight-based dose, and the patient’s weight was recorded inaccurately (plot alert: that’s what happened!)
I want to focus on the level of precision, though. How many significant digits should we present to our EHR user? Sure, there are mathematical and statistical rules about levels of significance and proper rounding, yet I don’t believe we need those. Like many things in life, it can be difficult to define the proper number of significant figures, but I know it when I see it.
Can we all agree that we’re probably OK to warn a physician that she may be about to dose a med at 45x the safe dose? 45x the safe dose! That, in my professional opinion, is pretty darn high. I wonder if 45x the safe dose makes more of an impression than 4,500 percent above the safe dose. Maybe yes, maybe no. But telling a doc that she’s 4,526 percent above the safe dose just seems silly to me.
For those of you who haven’t worked extensively with physicians, allow me to share an observation (maybe even an insider observation): physicians are born and bred to be cynical. We just are. My rationale for this statement will be a future blog post, but for now, just go with me. I think that often (not always, but often) doctors are looking to discount the information we provide in the EHR. And when we tell them that the dose of a medicine is 4,526 percent too high or that the max safe dose is exactly 1.9457 units, they appropriately scoff. And scoffing at the EHR is not good for anyone, believe you me.
Extensive observation (i.e. I recently bought air fresheners on Amazon.com) indicates to me that modern software doesn’t typically use absolute values for time any more. For instance, my photo app doesn’t tell me that I took this picture 582 days ago (although I did!) And my e-mail system speaks of days (<60), and months (2-24), and years (>=2) in a flexible, understandable, intuitive, and scalable way.
It’s time we bake appropriate numerical precision into all aspects of our EHR software. Who’s with me?
Craig Joseph, MD, is the Chief Medical Officer at Avaap where he works with healthcare leaders to implement and optimize EHRs in order to increase physician satisfaction, improve efficiency, and ensure full value of the technology.

